What to do in an emergency
 In an emergency?
In an emergency?
If you're with someone who needs medical help, call 999 and tell the responders everything you know about the drugs taken, it could save their life. If an ambulance comes and you have any drugs left, hand them over to the crew as it may help. In most circumstances they won't tell the police.
Should you ever need to help someone who’s having a bad reaction, here’s what you need to know:
What to look out for
If someone is having a bad time on drugs they may be:
disorientated, hallucinating, uncoordinated or panicky
overheated and dehydrated
struggling or unable to stay awake
having difficulty with breathing
What to do
The first things you should do are:
look at the surroundings and make sure you are safe
stay calm and be reassuring - don’t scare them or chase after them
try to find out what drugs they’ve taken
stay with them
If they are disorientated, hallucinating, uncoordinated or panicky you should:
sit them in a quiet and calm room
keep them away from crowds, bright lights and loud noises
tell them to take slow deep breaths
stay with them
If they are struggling or unable to stay awake you should:
sit them in a quiet place and keep them awake
not scare them, shout at them or shock them
not give them coffee to wake them up
not put them in a cold bath to wake them up – this wastes time and there’s a risk of drowning
If they are unconscious or having difficulty breathing you should:
immediately phone for an ambulance (call 999)
place them into the recovery position
stay with them until the ambulance arrives
if you know what drug they’ve taken tell the ambulance crew immediately, it might them get the right treatment faster
if you know they have taken an opioid and there is naloxone available, use it following the instructions on it. Find out more about naloxone here.
Recovery position
Follow the NHS guidance here.
By placing someone in the recovery position, you’re making sure that they are still breathing and can breathe easily, as it’s not unusual for someone who has become unconscious to swallow their tongue. You’re also making sure that if they vomit, it won’t block their airway and choke them.
Open their airway by tilting the head and lifting their chin. Lie them on their side and straighten their legs.
Place the arm nearest to you at right angles to the body. Get hold of the far leg just above the knee and pull it up, keeping the foot flat on the ground. Place their other hand against their cheek.
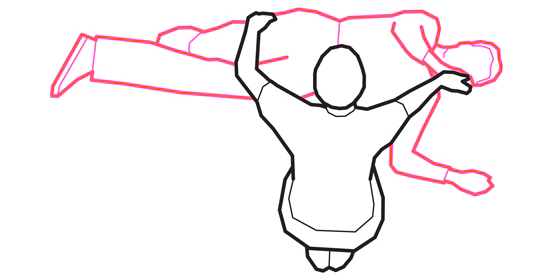
Keep their hand pressed against their cheek and pull on the upper leg to roll them towards you and onto their side.
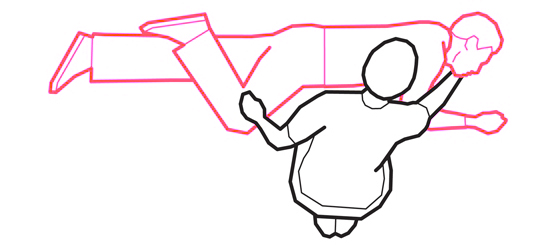
Tilt the head back so they can breathe easily.
Make sure that both the hip and the knee of the upper leg are bent at right angles.
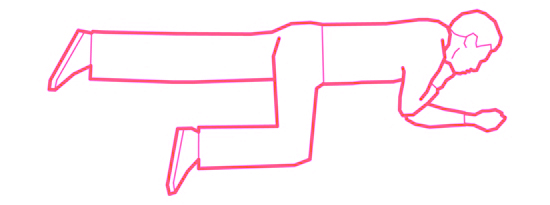
If they have stopped breathing
Immediately phone for an ambulance (call 999)
Start CPR (stands for cardio-respiratory resuscitation). When you call 999 they’ll give you instructions but you should start straight away. You can learn more about how to do CPR here.
If you know they have taken an opioid and there is naloxone available, use it following the instructions on it. Find out more about naloxone here.
What happens in A&E
In A&E the doctors and nurses will treat the person as best as they can. This may involve giving an antidote or treatment to counteract the effect of the drugs.
You can help by telling the ambulance crew, the doctors and nurses all you know about what drug(s) the person had taken, if they’d been drinking, and if they have any medical conditions. If there are still some of the drugs left, hand them over so they can find out what's in them.
Providing this information will help them give the person the right treatment without delay. In most circumstances they won’t tell the police, the person’s family or others not involved in their clinical care, that the person has been taking drugs.
Did you know?
999 is the number for the emergency services in the UK, but you can also call 112 for help
112 is the single emergency telephone number for anywhere in Europe
Naloxone - an antidote to opioid overdose
Naloxone is an emergency antidote to opiate overdose. It counteracts the effects of opioid drugs (such as heroin, methadone and fentanyl) and reverses the life-threatening effects of an overdose.
If you think someone has overdosed, you need to call an ambulance straight away so that expert help is immediately on its way.
Local services can make naloxone available, alongside training on how to use it, so that it can be supplied to people who might need it, such as drug users, their family and friends.
It’s normally very easy for people to use naloxone if they’ve had simple training. Overdose and naloxone training normally provides advice on:
how to recognise a possible opioid overdose
how to check for depressed or absent breathing
how to put the person in the recovery position (see diagram above) and call for an ambulance
how to provide CPR (this is essential if someone has stopped breathing)
how to use naloxone
Any training should give clear advice about building up the dose in stages as needed.
If it looks like the person is not breathing at all, or their heart has stopped, they will need further first aid before the ambulance arrives. The affected person will probably need mouth to mouth resuscitation and chest compressions (CPR). They might still benefit from a naloxone injection, but this mustn’t delay starting the required CPR.
Most overdose situations will need an ambulance to be called, the person put in the recovery position (please see this NHS first aid guide), naloxone injected, and someone to stay with the affected person until professional help arrives.
Naloxone works to reverse opioid overdose for only a short period of time. Even when the naloxone does work first time, you will still need to keep an eye on the person until the ambulance arrives, and during this time you may need to top up the naloxone more than once to keep the person awake and breathing adequately. An ambulance should always be called and someone should stay with the person until the ambulance arrives.
For more information about first aid, see the NHS Choices First Aid web page
What to do if you think someone may have alcohol poisoning
What alcohol poisoning is
Most people do not drink in a way that leads to alcohol poisoning but there is always a risk when people drink a lot of alcohol at one time. There is also a risk if you drink alcohol with sedative medication or drugs like benzodiazepine. This information could save the person’s life.
You can get alcohol poisoning (sometimes known as alcohol overdose) if you drink a lot of alcohol, particularly if you drink it over a short space of time (binge). Alcohol poisoning happens when your body can not process the amount of alcohol you have drunk.
The amount of alcohol that can lead to alcohol poisoning is different for different people. It depends on things like body size and general health.
If you drink as much as 12 units or more, especially during a short space of time, you can be at risk of alcohol poisoning. For some people, especially children and young people, drinking less than this can lead to alcohol poisoning.
Anybody can get alcohol poisoning, but you might be more at risk If you are quite new to drinking alcohol and have not experienced its’ toxic effects before, or if you drink heavily after you have had a break from drinking for a while.
Alcohol poisoning affects your breathing, heart rate and gag reflex (so you are more likely to choke) and puts you at risk of a coma and of death.
If you drink a lot of alcohol and also take drugs you may become ill or overdose from a combination of drugs and alcohol
What to look out for
A person with alcohol poisoning may show some or all of the signs below:
confusion
vomiting
seizures (fits)
slow breathing
pale or bluish skin
cold and clammy skin
unconsciousness
What to do
The first things you should do are
Call 999 immediately and ask for an ambulance
Stay calm
Reassure the person and don’t shout at them
Try to find out how much they have had to drink and if they have taken any drugs or medication
Don’t let them drink any more alcohol
Stay with the person until the ambulance arrives and watch them carefully
If they are drowsy
Help the person to stay upright and awake if possible
Help the person to sip water if they can swallow
DO NOT make the person vomit. This is because their gag reflex may not be working and vomiting can lead to them choking.
Don’t give them coffee to wake them up as this can cause dehydration
Don’t put them in a cold bath to wake them up – this wastes time and there’s a risk of drowning
Stay with the person until the ambulance arrives and watch them carefully
If the person is unconscious
Call the ambulance immediately
Place the person on their side with their ear to the ground with a cushion under their head. See recovery position.
Stay with the person until the ambulance arrives and watch them carefully
When the ambulance crew arrive, tell them what you know about how much the person has had to drink and their condition. If they have also taken drugs, tell the ambulance crew everything you know about the drugs taken it might them get the right treatment faster


